Exercises for prolapse can help women to reduce prolapse symptoms and improve prolapse support. This article teaches you how to do prolapse exercises that get you results.
Read on now to learn:
- What is a prolapse?
- What are the symptoms of prolapse?
- Can pelvic floor exercises or kegels help manage a prolapse and stop it from worsening?
- How to do prolapse exercises that work?
- Important mistakes to avoid when doing pelvic floor exercises for prolapse
- When to seek professional help for prolapse exercises
This information on prolapse exercises applies to women with uterine prolapse, bladder prolapse, bowel and rectal prolapse.
What is a Prolapse?
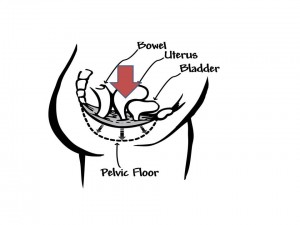
- Vaginal prolapse occurs when the vaginal tissues and supporting structures inside the pelvis become weak. This allows the pelvic organs that sit close to the vagina to bulge into the vaginal walls.
- Bladder prolapse (cystocoele or prolapsed bladder) involves the bladder bulging into the front wall of the vagina
- Bowel prolapse (rectocoele) involves the bowel bulging into the back wall of the vagina
- Uterine prolapse involves the uterus losing its support and moving down into the vagina
- Rectal prolapse involves the walls of the rectum protruding out of the anus.
Prolapse Exercises e-Book
International best selling prolapse exercise guide for women with prolapse and after prolapse surgery.
Prolapse Exercises teaches you how to:
- Exercise safely after prolapse surgery
- Reduce your risk or repeat prolapse
- Avoid unsafe exercises
- Choose pelvic floor safe exercises
- Reduce your risk of prolapse worsening
- Improve prolapse support
- Increase your strength and fitness
- Strengthen your core
- Lose weigh
Symptoms of Prolapse
A prolapse can produce a variety of symptoms, and some of these prolapse symptoms depend on the type and/or severity of the prolapse.
Symptoms of prolapse may include:
- Feeling heaviness in the vagina;
- Dragging sensation in the vagina or pelvis;
- Lump or bulge at the entrance of the vagina;
- Difficulty inserting tampons;
- Wind escaping from the vagina with intercourse; and
- Difficulty emptying the bladder and/or bowel.
Can Exercises for Prolapse Help?
Yes, specific pelvic floor exercises for prolapse can assist women with prolapse management in the following ways.
1. Symptom relief
Many women report that doing pelvic floor exercises regularly helps alleviate their prolapse symptoms. This is often the case for women with mild to moderate prolapse. When the prolapse extends beyond the entrance of the vagina, pelvic floor exercises may not improve a woman’s symptoms however this doesn’t mean pelvic exercises are not beneficial.
2. Prolapse support
The pelvic floor muscles are designed to assist in the support of the pelvic floor including the pelvic organs susceptible to prolapse (bladder, vagina and rectum). It makes sense that improving pelvic support with strong, firm well functioning pelvic floor muscles will help to manage a prolapse. If the pelvic floor muscles become strong enough to withstand the pressure associated with everyday activities, then a well functioning pelvic floor may even help to prevent the prolapse worsening.
3. Reduced straining
When the pelvic floor muscles are working as they should, they assist bowel emptying and lessen the need to strain. Women can benefit from knowing correct bowel emptying technique to use to avoid straining as part of their overall prolapse management strategy. Well functioning pelvic floor muscles can help empty the bowels and reduce straining.

For more information about safe prolapse exercises please refer to Inside Out – the essential women’s guide to pelvic support. This easy to read book provides comprehensive professional guidelines for how to improve pelvic support with prolapse exercises.
How to do Exercises for Prolapse?
Pelvic floor exercise are an inwards lift and squeeze of the pelvic openings (urethra, vagina and anus). It is then important to fully relax your pelvic floor muscles and allow them time to rest between each exercise or contraction.
Check you are using the right muscles by:
- Feeling a lift and squeeze inside the area where you sit; and
- Feeling a sensation of letting go when you relax these muscles.
Tips for exercising pelvic floor muscles with a prolapse:
- Practice your prolapse exercises earlier rather than later in the day;
- Position yourself where you can best feel your pelvic floor muscles working, perhaps lying down to reduce the downward pressure on your pelvic floor and your prolapse; and
For further details on how to do exercises for prolapse, please refer to our daily prolapse exercise guidelines.
Mistakes to Avoid With Exercises for Prolapse
Some mistakes are commonly made when women attempt to exercise their pelvic floor muscles.
These include:
- Bearing down or straining rather than lifting up the pelvic floor muscles with exercise;
- Breath holding when contracting the pelvic floor muscles;
- Pulling in the upper abdominal muscles strongly with the exercise; and
- Squeezing the buttocks or inside thigh muscles.
When to Seek Professional Help With Exercises for Prolapse?
If you are having difficulty with your prolapse exercises, it is advisable to seek treatment with a Pelvic Floor Physiotherapist or a Continence Nurse Advisor. These health professionals can assist with common problems encountered when exercising the pelvic floor such as;
- Difficulty feeling your pelvic floor muscles lifting or relaxing;
- Problems breathing and activating at the same time;
- Lack of confidence in performing the correct action; or
- Lack of progress with your pelvic floor exercises.
‘Exercises for Prolapse’ is by Pelvic Floor Physiotherapist Michelle Kenway. Michelle is the author of Inside Out – the essential women’s guide to pelvic support along with Dr Judith Goh, Urogynaecologist.







